Navigation Drug
Development of Navigation Drug for cancer surgery using activatable fluorescent probe
In cancer surgery, complete removal of the cancer cells is essential, and visualization of minute cancer is a major challenge. Goryo Chemical, Inc. has successfully developed an activatable fluorescent probe (designated as a navigation drug: ND) which can visualize minute target sites with high-sensitivity and selectively.
 Significance and Merit
Significance and Merit
According to an overseas report, approximately 25% of patients receiving breast cancer surgery (partial breast excision) require repeated surgery due to recurrence 1). One possible cause is that all the cancer cells were not removed during initial surgery. In order to decrease the amount of cancer cells that remain behind, progress in developing techniques to visualize minute cancer sites, which are difficult to differentiate from normal tissue, during surgery, has been made.
Currently, common preoperative diagnostic techniques to identify minute cancer sites include PET (position emission tomography), SPECT (single-photon emission computed tomography), and MRI (magnetic resonance imaging). In recent years, a certain degree of success has been reported in the use of FIGS technology to detect target cancer sites by fluorescent probes during surgery. However, detecting millimeter sized cancer sites has been found to be difficult. Consequently, Goryo Chemical, Inc., utilizing know-how from an exclusive manufacturer of fluorescent probes, has developed technology (ND) to visualize minute cancer by activatable fluorescent probes. Currently, we are seeking to apply this ND to clinical use, and have proceeded to clinical testing. For this technology guidance has been provided by Prof. Urano, et al., of the University of Tokyo, and many articles have been published (please refer to the references in each section GCP-001, GCP-002, and GCP-003).
If visualization of minute cancer tissue during surgery can be realized, accuracy in the removal of cancer can be improved, and the amount of cancer that remains behind can be minimized to zero. In addition, judgment using ND can be quickly performed in as little as 5 minutes. If this technology can be used for intraoperative rapid diagnosis, a reduction in surgical time and the rates of repeat surgery and recurrence are expected to decrease, leading to a decrease in patient burden.
The projects are under the supervision of Prof. Yasuteru Urano (Laboratory of Chemical Biology and Molecular Imaging, Graduate School of Medicine, The University of Tokyo, Laboratory of Chemistry and Biology, Graduate School of Pharmaceutical Sciences, The University of Tokyo) and Prof. Yasuyuki Seto (Department of Gastrointestinal Surgery, Graduate School of Medicine, The University of Tokyo).
Reference
-
1)G. E. Moore, W. T. Peyton, L. A. French, W. W. Walker (1948)
Neurosurg. 5 (4): 392–398. DOI:10.3171/jns.1948.5.4.0392
 What is a Navigation Drug?
What is a Navigation Drug?
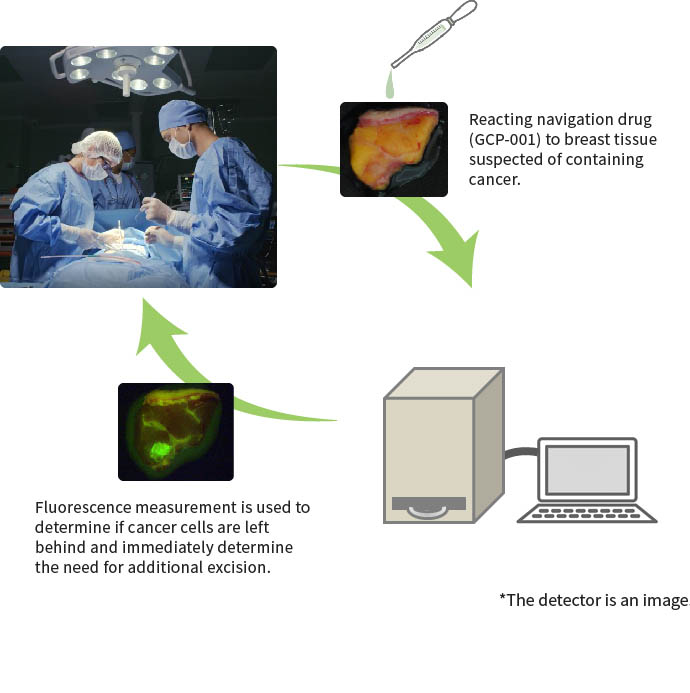
A navigation drug (ND) is a new cancer detection technology suggested by Goryo Chemical, Inc. The purpose of a ND is to increase precision in surgery, and decrease cancer cells remaining after visualization of cancer tissue by activatable fluorescent probes, and to navigate (guide) the surgery. For example, in vitro diagnostic breast cancer detection probe, the probe is applied to the surgically excised sample, and cancer sites are detected using the dedicated equipment in approx.
GCP-001 is applied to breast cancer tissue and normal breast tissue, and change in fluorescence is measured over time. Reaction occurs in 5 minutes, and a significant increase in fluorescence is observed in breast caner tissue. ND is indicated to be effective for visualization of cancer sites.
 What is Activatable Fluorescent Probe?
What is Activatable Fluorescent Probe?
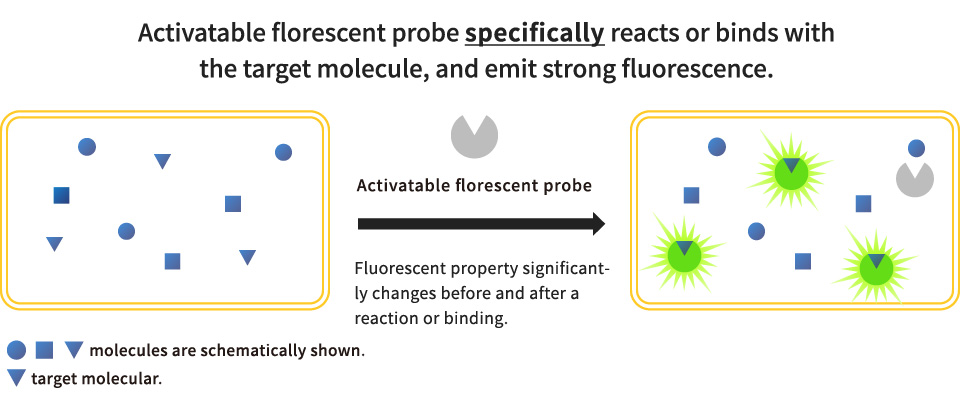
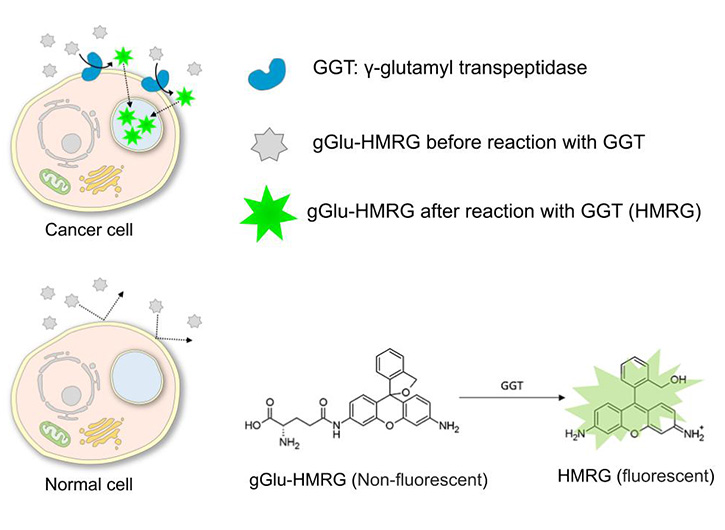
“The fluorescent probe molecule undergoes a quenching process rendering it non-fluorescent. However, when the probe reacts and binds with the observation target molecule. 1)” In other words, the fluorescence characteristics of the fluorescent probe molecule significantly change before and after reaction with the target molecule (Fig.2).
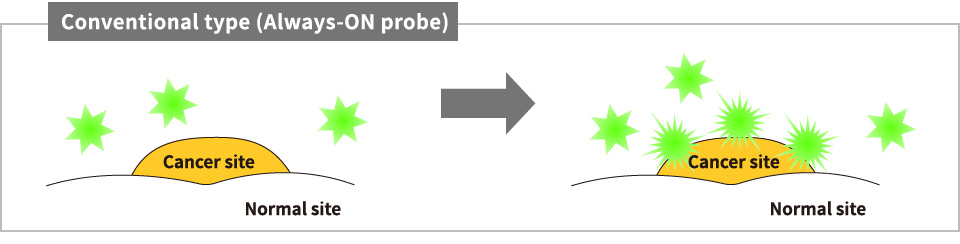
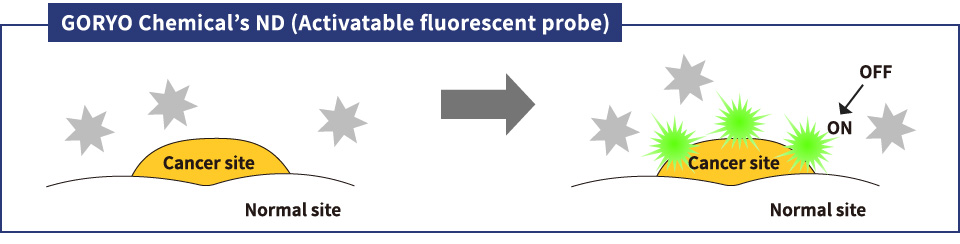
Fluorescents probes have been widely used at the clinical site up to now, and have high safety and low toxicity. An activatable fluorescent probe by Goryo Chemical, Inc. is designed to detect enzymes which have a confirmed and specific advanced expression in individual cancer cells. When an activatable fluorescent probe is used, detection of minute amounts of cancer in a cancer site, which is conventionally difficult, can be expected (Fig. 5). Goryo Chemical, Inc. has successfully developed activatable fluorescent probes as ND (GCP-001, 002, 003) which can be used in the clinical site. Fig. 2 and Fig. 3 modified based on the figure provided by Prof. Yasuteru Urano.
Reference
- 1)Highly Sensitive and Intraoperative Detection of Tiny Tumors with Novel “Activatable“ Fluorescence Probes
Yasuteru Urano
https://www.jstage.jst.go.jp/article/yakushi/132/4/132_4_397/_pdf/-char/ja
 Breast Cancer Detection GCP-001 (gGlu-HMRG)
Breast Cancer Detection GCP-001 (gGlu-HMRG)
An activatable fluorescent probes for breast cancer detection
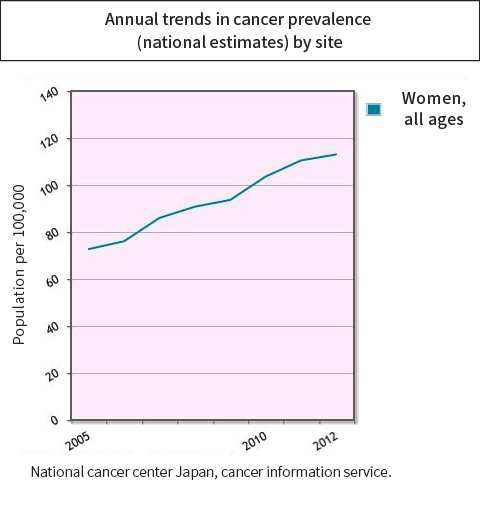
1. About breast cancer
In Japan, breast cancer has the highest frequency among cases of cancer among women, with approximately 72,000 new cases each year, and this number increases every year (study by the National Cancer Center 1) Graph 1).
Cases with localized cancer are considered to have higher chance of permanent cure by surgical treatment (Clinical Practice Guidelines: Breast Cancer 2015), and surgical excision are currently performed.
*Permanent cure: Condition in which symptoms are completely recovered, and further treatment at the hospital is not needed
2. Reaction of gGlu-HMRG with GGT
gGlu-HMRG is a green fluorescent probe in which the substrate of GGT is bound to the fluorophore HMRG (hydroxymethyl rhodamine green). Although it does not emit fluorescence before GGT reaction, once hydrolyzed by the enzyme activity of GGT, results in a green fluorescence emission. HMRG shows cell membrane permeability and accumulates in the lysosomes due to electron gradient, resulting in a spot-like strong green fluorescence image.
Gamma-glutamyl transferase (GGT) is a membrane-bound enzyme. Enhancement of GGT expression and enzyme activity has been reported in breast cancer cells. (, and it is involved in biosynthesis of antioxidant glutathione.)
3. Clinical data
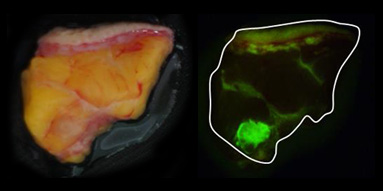
According to a clinical study by a group centered at Kyushu University Beppu Hospital, GCP-001 (gGlu-HMRG) has been shown to have high intensity and specificity for specific cancer sites.
GCP-001 is applied to excised breast tissue and allowed to react for 3 minutes. Fluorescence is then detected and measured. An area where strong fluorescence is detected in the breast tissue (upper right image), and a tumor in almost the same area was confirmed by magnification of the tissue sample (bottom right image, tumor stained green). Cancer specificity of GCP-001 is demonstrated, indicating the usefulness as a ND.
(Provided by: Dr. Ueo, Department of Breast Surgery, Saiseikai Fukuoka General Hospital)
Details link:http://www.nature.com/articles/srep12080
4. References
- 1)National cancer center Japan, cancer information service http://ganjoho.jp/reg_stat/
 Esophageal cancer detection GCP-002 (EP-HMRG)
Esophageal cancer detection GCP-002 (EP-HMRG)
An activatable fluorescent probe for esophageal cancer detection
1. About esophageal cancer
Each year in Japan, more than 20,000 contract esophageal cancer, and more than 10,000 die. Compared with other cancers of the alimentary canal, prognosis is extremely poor due to metastasis to the lymph node during the early stage, infiltration into surrounding organs is common, extensive surgical invasion, high frequency of mortality during surgery, postoperative complications, and recurrence 1, 2).
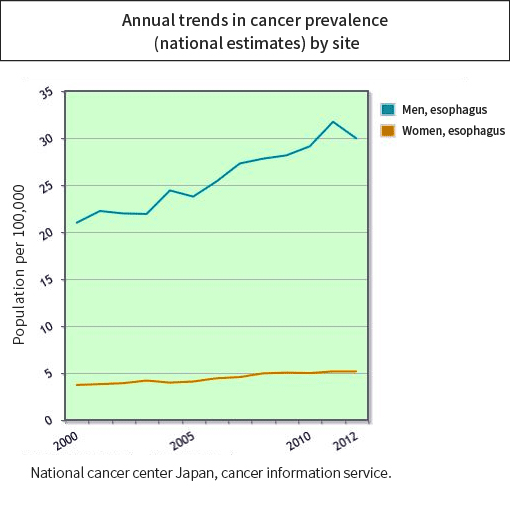
In Japan, there is an increasing trend for esophageal cancer in men, while it has remained level in women. By gender, a higher frequency is reported for men (study by the National Cancer Center (Graph 2)).
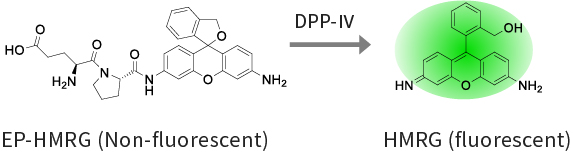
2. Reaction of EP-HMRG with DPP-Ⅳ
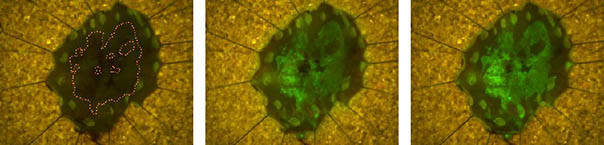
EP-HMRG is a green fluorescent probe in which the substrate of DPP-Ⅳ is bound to the fluorophore HMRG (hydroxymethyl rhodamine green). Although it does not emit fluorescence before DPP-Ⅳ reaction, once hydrolyzed by the enzyme activity of DPP-Ⅳ, results in a green fluorescence emission. HMRG shows cell membrane permeability and accumulates in the lysosomes due to electron gradient, resulting in a spot-like strong green fluorescence image. Dipeptidyl peptidase-Ⅳ (DPP-Ⅳ) is a membrane-bound enzyme. Enhancement of DPP-Ⅳ expression and enzyme activity has been reported in esophageal cancer3).
3. Clinical data
In a clinical study at the University of Tokyo Hospital, EP-HMRG was applied to an excised human esophageal cancer ESD sample in order to identify cancer sites. As a result, EP-HMRG was shown to have high intensity and specificity.
Data were provided by Prof. Yasuyuki Seto.
Details link:http://www.nature.com/articles/srep26399
4. References
- 1)National cancer center Japan, cancer information service http://ganjoho.jp/reg_stat/
- 2)The 3rd Guidelines for Diagnosis and Treatment of Carcinoma of the Esophagus KANEHARA & CO., LTD.
- 3)H. Onoyama, M. Kamiya, Y. Kuriki, T. Komatsu, H. Abe, Y. Tsuji, K. Yagi, Y. Yamagata, S. Aikou, M. Nishida, K. Mori, H. Yamashita, M. Fujishiro, S. Nomura, N. Shimizu, M. Fukayama, K. Koike, Y. Urano, Y. Seto (2016)
Sci. Rep. 6: 26399 DOI: 10.1038/srep26399
 Pancreatic fistula detection GCP-003 (gPhe-HMRG)
Pancreatic fistula detection GCP-003 (gPhe-HMRG)
An activatable fluorescent probe for pancreatic fistula detection
1. About pancreatic fistula
Pancreatic fistula is a postoperative complication where pancreatic juice secreted from pancreas leaks into the abdominal cavity after surgery targeting the pancreas and surrounding organs. Digestive enzymes which dissolve protein, fat, and sugar are contained in the pancreatic fistula, and also cause infection, may lead to serious symptoms in abdominal cavity such as damaged blood vessels, and may cause bleeding by autodigestion action.
For example, excision of the pancreas in cases of pancreatic cancer is very difficult, and the occurrence rate of pancreatic fistula is reported to be high rate (10-50 %) 1, 2, 3). The occurrence rate during stomach cancer surgery accompanied with lymph node dissection and splenectomy is also reported to be high (5-22 %) 4, 5, 6).
Occurrence of pancreatic fistula is high because it is difficult to confirm leakage of pancreatic juice during surgery, since it is colorless and transparent. Development of a method to confirm the presence of pancreatic fistula has strongly desired.
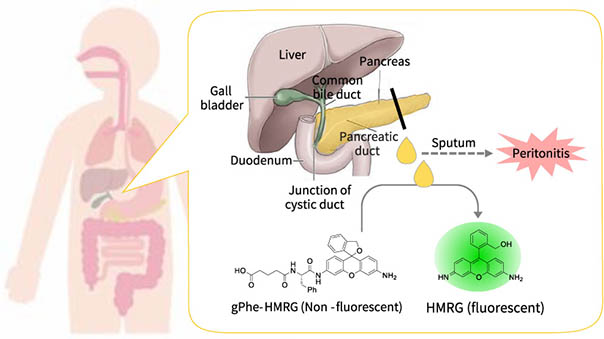
2. Reaction of gPhe-HMRG with chymotrypsinogen
The pancreatic juice detection probe (gPhe-HMRG and trypsin) itself is non-fluorescent, but when sprayed on pancreatic juice, it reacts with chymotrypsinogen contained in pancreatic juice to generate HMRG that emits strong fluorescence.
By measuring the fluorescence of HMRG, pancreatic juice can be detected.
3. References
- 1)Yeo CJ, Cameron JL, Sohn TA, Lillemoe KD, Pitt HA, Talamini MA, Hruban RH, Ord SE, Sauter PK, Coleman J, Zahurak ML, Grochow LB, Abrams RA (1997)
Ann Surg. 226 (3): 248-260. DOI: 10.1097/00000658-199709000-00004 - 2)Mckay A, Mackenzie S, Sutherland FR, Bathe OF, Doig C, Dort J, Vollmer CM Jr, Dixon E. (2006)
Br J Surg. 93: 929-936. DOI: 10.1002/bjs.5407 - 3)Fuks D, Piessen G, Huet E, Tavernier M, Zerbib P, Michot F, Scotte M, Triboulet JP, Mariette C, Chiche L, Salame E, Segol P, Pruvot FR, Mauvais F, Roman H, Verhaeghe P, Regimbeau JM (2009)
Am J Surg. 197: 702-709. DOI: 10.1016/j.amjsurg.2008.03.004 - 4)T. Sano, M. Sasako, S. Yamamoto, A. Nashimoto, A. Kurita, M. Hiratsuka, T. Tsujinaka, T. Kinoshita, K. Arai, Y. Yamamura, K. Okajima (2004)
J Clin Oncol. 22: 2767-2773. DOI: 10.1200/JCO.2004.10.184 - 5)H. Katai, K. Yoshimura, T. Fukagawa, T. Sano, M. Sasako (2005)
Gastric Cancer, 8: 137-141. DOI: 10.1007/s10120-005-0317-8 - 6)Y. Miki, M. Tokunaga, E. Bando, Y. Tanizawa, T. Kawamura, M. Terashima (2011)
J Gastrointest Surg. 15: 1969-1976. DOI: 10.1007/s11605-011-1628-1
Development scheme and product development status
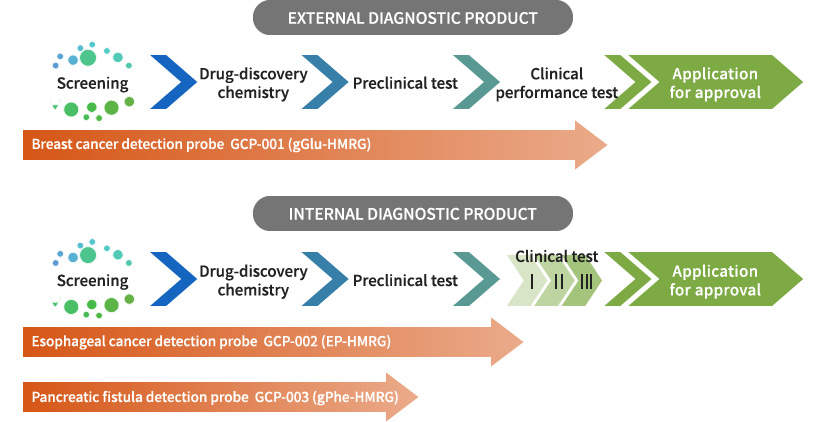
Goryo Chemical, Inc. is currently developing the three agents described above, seeking to provide these to the clinical site as navigation drugs for use during surgery as soon as possible.




 Contact Us
Contact Us
